Fertility Surgery for Women
The Center's physicians are experienced surgeons who routinely perform minimally invasive laparoscopic and hysteroscopic procedures, which require less recovery time than traditional “open” surgery.
Laparoscopy
Laparoscopy is a surgical technique in which the physician examines the abdomen and pelvis through a small incision in the navel. The physician inserts a thin fiberoptic tube with a camera called a laparoscope to see any fertility issues that are not detectable by a physical examination or ultrasound. Many conditions—such as tubal blockage, ovarian cysts, pelvic adhesions, uterine fibroids or endometriosis—can be treated by laparoscopy during the same surgery.
Hysteroscopy
Hysteroscopy is a surgical technique that allows the physician to examine the uterine cavity with a small scope inserted into the uterus. The physician is then able to remove fibroids, polyps and repair any scarring that may have resulted from prior uterine surgeries.
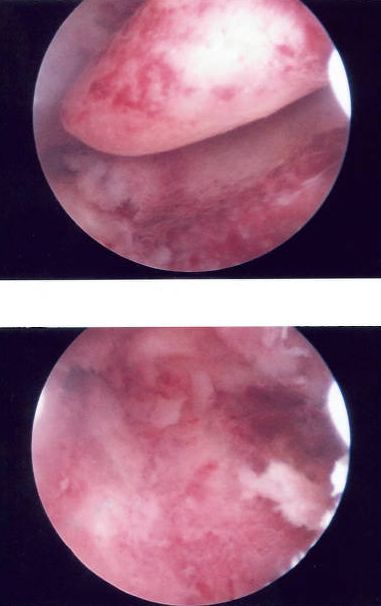
Above: Before-and-after images of a uterine polyp
removal using hysteroscopy
Robotic Surgery
The Center’s state-of-the-art equipment includes da Vinci surgical robots that allow surgeons to perform complex operations through small incisions—so-called “robotic surgery.”
Fertility Surgery for Men
CRM partners with the Center for Male Reproductive Medicine & Microsurgery of Weill Cornell Medical College, the first university center in the United States devoted exclusively to male infertility treatment. Our urologist colleagues have pioneered sperm-retrieval and microsurgical repair techniques that have allowed thousands of men to become fathers.
Surgical Repair
Male reproductive urologic microsurgeons can repair or remove anatomical obstructions such as congenital blockages or a prior vasectomy which prevent sperm from reaching the ejaculate. Microsurgery is also the method of choice to repair varicoceles (varicose veins in the scrotum). A varicocele is the most common cause of low sperm count and low testosterone.
Surgical Sperm Retrieval
For men with very low or no sperm count, surgeons locate and collect sperm for use in ICSI with an IVF cycle or to be frozen for future use. Most of these procedures, including micro-TESE (microscopic testicular sperm extraction, pronounced "tess-ee"), are performed in an outpatient setting.
Please contact a physician's office at the Center for Male Reproductive Medicine & Microsurgery of Weill Cornell Medical College for more information and to make an appointment.

